
Vol. XXI, No. 5, May 2021
- Editor's corner
- New esports concepts
- Is the current surge in attendance only a false dawn?
- Covid baby bust - 2020 births lowest since 1979
- The return to in-person dining and foodyism
- Understanding Covid -19 infection risk: indoor & outdoor transmission and masks
- A new type of transformational experience to drive in-person attendance
- TV celebrity chef raising the bar for eatertainment
Understanding Covid -19 infection risk: indoor & outdoor transmission and masks
On April 27th, the CDC issued new guidance on when and where fully vaccinated and unvaccinated people should wear masks. It issued the following chart on the risk of different activities.
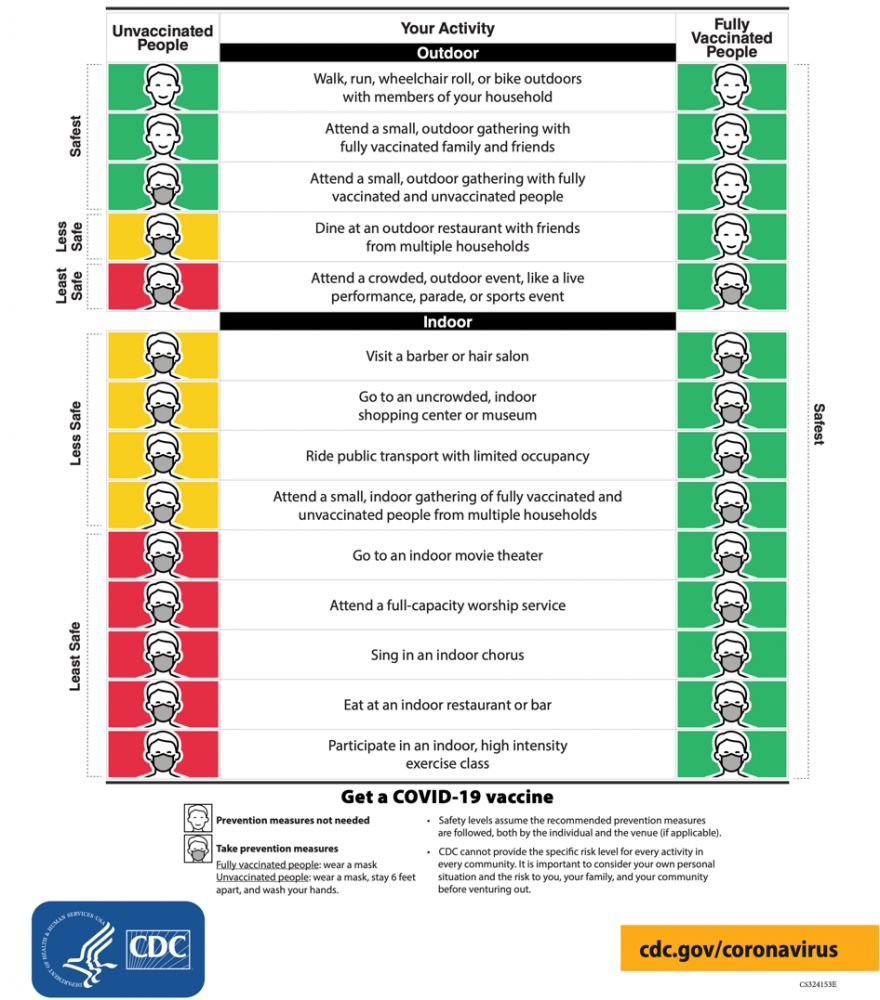

The revised recommendations include that fully vaccinated people can safely attend small, outdoor gatherings with fully vaccinated and unvaccinated people, and dine at outdoor restaurants with friends from multiple households without wearing a mask, but not without a mask at crowded, outdoor events like a concert, parade or sports event. They also said that unvaccinated people are safe (safest) without wearing a mask attending small, outdoor gatherings with fully vaccinated family and friends, but not unvaccinated people, or dining at an outdoor restaurant.

The recommendations in the chart can get somewhat confusing considering all the different combinations of indoor and outdoor activities with vaccinated and unvaccinated people. Here's a way to conceptual understand how the risk varies based on the circumstances.
Coronavirus is transmitted by airborne respiratory droplets. Airborne droplets from an infected person will drop to the ground quickly. The distance they will travel varies depending on whether the infectious person is talking softly, talking loudly, singing, yelling, sneezing, or coughing. One study found that droplets can travel further than six feet from just talking. Some studies have found that droplets can travel around 20 feet from coughing or sneezing. This is why it is important for the infectious person, who could be asymptomatic, and the other person near them, to both wear face coverings, as masks significantly reduce the transmission of droplets depending on their types and how snuggly they're worn. That is why universal mask-wearing has been so important, even if maintaining a "social distance" of six feet away from other people.
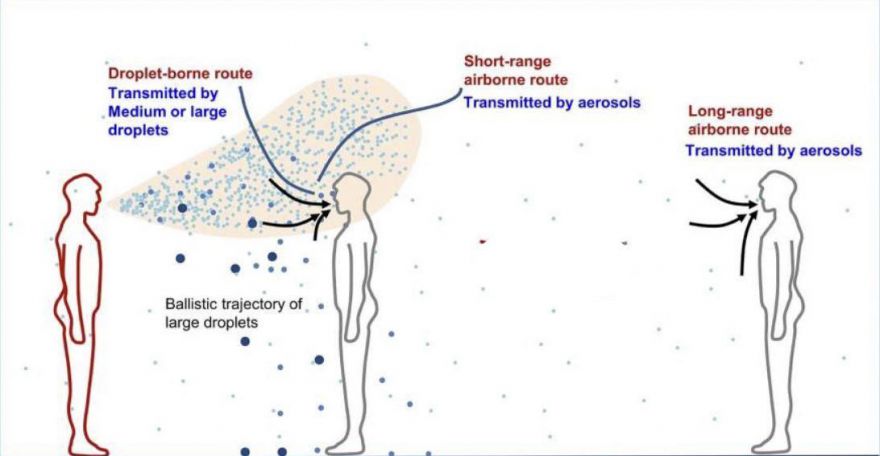
Covid-19 is transmitted by droplets and aerosols
In addition to droplets, infectious people transmit smaller virus-carrying atomized particles, aerosols that are quite light and then float in the air and linger suspended in the air for several hours far away from their source, especially in poorly ventilated spaces. A recent MIT study found that socially distancing indoors may provide a "false sense of safety." The study found that people who maintain 60 feet of distance from others indoors are no more protected from infection than if they are socially distanced by six feet. The research said that the air an infectious person breathes out contains infected aerosols even if they are wearing a mask (no mask totally filters out aerosols). Those aerosols then rise and come down elsewhere in the room, so you are more exposed to the average background of infected aerosols than you are to the person at a distance. The higher the concentration of aerosols and the longer you spend in a space increases your infection risk (long enough to inhale the minimum infectious dose required for infection).
A good analogy to understand this is secondhand smoke. If you are at a restaurant bar with 50 people in a separate smaller room from the dining room, and one person has been smoking for some time, you will smell secondhand smoke and breathe it in no matter where you are in the bar. If you then move to the main dining room, which is a much larger room and there are 50 people with one smoking, the concentration of secondhand smoke will be much less. Of course, the air filtration and ventilation rates affect the concentration of secondhand smoke.
If you are outdoors near a person smoking, and they aren't close and directly upwind from you, it is unlikely you will breathe any secondhand smoke, as the smoke is quickly dispersed. That is why the infection risk is so much lower outdoors as long as it isn't a crowded situation of long duration, such as sitting in a seat at an outdoor sports event.
If you want to reduce your risk of infection, the best strategy is to assume someone, where you are with other people, is smoking and you are averse to secondhand smoke. Even the mask you're wearing won't totally filter it out. (The CDC recently reported you can also catch Covid-19 when droplets or aerosols come in contract with your eyes.) So, you don't want to spend a long time in a place where there is secondhand smoke. That will almost always be in an indoor space.
Now, if you're fully vaccinated, your risk of infection is significantly reduced by more than 90% for the mRNA vaccines. That is why the CDC considers it so safe for you to be outdoors with other people even if they are not vaccinated, as their infectious aerosols, their secondhand smoke, is unlikely to reach you. The vaccine further reduces your infection risk even if it does reach you.
Getting back to the MIT research, Martin Bazant, one of the researchers, said, "What our analysis continues to show is that many spaces that have been shut down, in fact, don't need to be. Often times the space is large enough, the ventilation is good enough, the amount of time people spend together is such that those spaces can be safely operated even at full capacity and the scientific support for reduced capacity in those spaces is really not very good. I think if you run the numbers, even right now for many types of spaces you'd find that there is not a need for occupancy restrictions."
The CDC guidance and MIT research mean that a 50,000-square-foot, mostly all open, family entertainment center with high ceilings and good air ventilation might be reasonably safe for a 2-hour-stay wearing masks. At the same time, a small, crowded birthday party room is probably not very safe for 45 minutes, even for vaccinated people wearing masks. Playing miniature golf outdoors with friends, some of whom aren't vaccinated, should be safe for vaccinated people not wearing a mask, but unvaccinated people should wear face coverings.
The MIT research offered a handy online risk-assessment calculator to help people better understand what factors in a given indoor setting may increase their risk for catching the coronavirus.
Of course, the bottom line for all this is that regardless of whether fully vaccinated or not vaccinated, the safest strategy is to wear a facemask.
Additional reading - see our CEO's blog:
Vol. XXI, No. 5, May 2021
- Editor's corner
- New esports concepts
- Is the current surge in attendance only a false dawn?
- Covid baby bust - 2020 births lowest since 1979
- The return to in-person dining and foodyism
- Understanding Covid -19 infection risk: indoor & outdoor transmission and masks
- A new type of transformational experience to drive in-person attendance
- TV celebrity chef raising the bar for eatertainment



