
Vol. XXI, No. 8, September 2021
What they fail to explain about vaccines, Delta, and masks
by Randy White, CEO White Hutchinson Leisure & Learning Group
It's disappointing that the Federal government, especially the CDC, and the press are doing such a poor job of informing us about the factors that affect the risk of catching the new more dangerous Delta variant and what we really need to do to stay as safe as possible. The Delta variant is now estimated to account for more than 99% of all Covid virus strains circulating in the U.S. The Delta variant is far more contagious than the original Alpha Covid virus. Scientists say that with Delta, an infection can happen in less than five minutes after close contact with an infected person versus 15 minutes for the original Alpha virus. A new study in the journal The Lancet Infectious Diseases found that people who contracted the Delta variant were about twice as likely to require hospitalization as those who contracted the Alpha variant.
Disclaimer: I'm not a doctor, immunologist, scientist, or medical expert. What follows is a simplified summary of all the research I've reviewed, integrated into a not too technical and hopefully understandable explanation.
Vaccines don't protect you from getting infected
One of the most important things to understand is that the Covid vaccines do not protect you from getting infected. Most vaccines don't. Instead, they lower the probability of getting infected, and if infected, they protect you from getting seriously ill or ending up in the hospital. Most infections of vaccinated people are believed to be asymptomatic (no symptoms) or very mild. The mRNA vaccines have proven to be very effective; the J&J is a little less so. According to the Centers for Disease Control and Prevention (CDC), approximately 99.5% of COVID-19 deaths in the United States are among unvaccinated people.
How Covid is transmitted
Airborne respiratory droplets transmit Covid. Airborne droplets from an infected person will drop to the ground quickly. The distance they will travel varies depending on whether the infectious person is talking softly, talking loudly, singing, yelling, sneezing, or coughing. One study found that droplets can travel further than six feet from just talking. Some studies have found that droplets can travel around 20 feet from coughing or sneezing. Therefore, it is important for the infectious person, who could be asymptomatic, and any people near them, to wear face coverings, as masks significantly reduce the transmission of droplets depending on their types and how snuggly they're worn. That is why universal mask-wearing is important, even if maintaining a "social distance" of six feet away from other people.
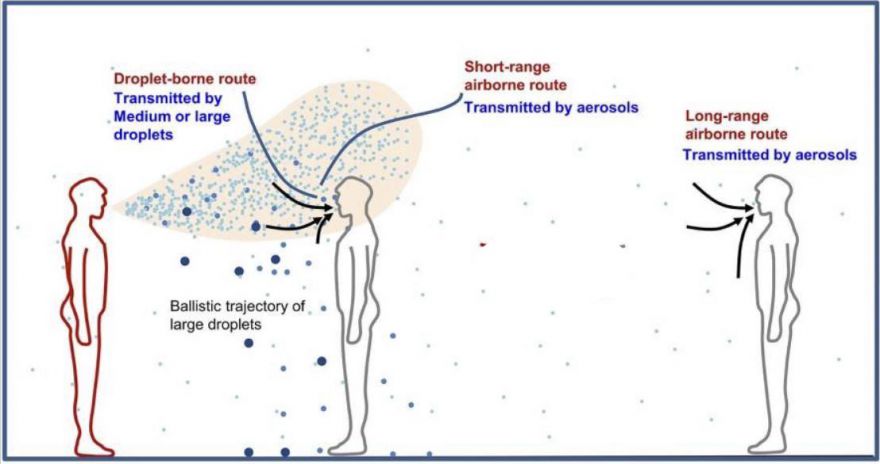
Covid-19 is transmitted by droplets and aerosols
In addition to droplets, infectious people transmit smaller virus-carrying atomized particles, aerosols that are quite light and then float in the air and linger suspended in the air for several hours faraway from their source, especially in poorly ventilated spaces. A recent MIT study found that socially distancing indoors may provide a "false sense of safety". The study found that people who maintain 60 feet of distance from others indoors are no more protected from infection than if they are socially distanced by six feet. The research found that the air an infectious person breathes out contains infected aerosols even if they are wearing a mask (no mask totally filters out aerosols). Those aerosols then rise and come down elsewhere in the room, so you are no less exposed to the average background of infected aerosols than you are to the person at a close distance. The higher the concentration of aerosols and the longer you spend in a space increases your infection risk (long enough to inhale the minimum viral dose required for infection).
One reason Delta is so highly infectious is that an infected person's droplets and aerosols have much higher concentrations, hundreds of times more of the virus than the original coronavirus. Studies have also found that asymptomatically infected vaccinated people shed just as many Delta viruses as an infected unvaccinated person. This is why even vaccinated people who are together should wear masks.
A good analogy to understand this is secondhand smoke. If you are at a restaurant bar with 50 people in a separate smaller room from the dining room, and one person has been smoking for some time, you will smell secondhand smoke and breathe it in no matter where you are in the room. If you then move to the main dining room, which is a much larger room, and there are 50 people with one smoking, the concentration of secondhand smoke will be much less. Of course, air filtration and ventilation rates affect the concentration of secondhand smoke.
If you are outdoors near a person smoking, or they aren't close and directly downwind from you, it is unlikely you will breathe in any secondhand smoke. That is why the infection risk is lower outdoors as long as it isn't a crowded situation of long duration, such as sitting in a seat at an outdoor sports event.
How immunity works with prior infection or vaccination
If you have had a prior Covid infection or are vaccinated, your immune system was prompted to develop trained B-cells that quickly produce antibodies that recognize and specifically target the Covid virus, known as adaptive immunity. Neutralizing Covid virus particles from the environment is the sole responsibility of those antibodies in our respiratory, GI, and ocular secretions — our "frontline" defensive antibodies in our saliva, tears, nasal secretions, and pulmonary mucus. When we are exposed to airborne virus particles, these antibodies attach to the spike protein of Covid, physically preventing it from latching on to what is called the ACE2 receptors on the surface of our respiratory epithelium and gaining entry to those cells to cause an infection. However, if we are exposed to so many virus particles that all the antibodies in these secretions have already attached themselves to virus particles, and we continue to be exposed to new particles faster than more antibodies are transported into these secretions, then our antibody defense gets overwhelmed, we inhale or come in contact with more virus particles than we can neutralize, and we get infected. In other words, the viral load exceeds the capacity of the antibodies to neutralize them.
Once infected, the virus invades our cells to replicate. That's what your circulating neutralizing antibodies fight. They attach to the spike proteins of the newly created virus particles to prevent them from infecting other cells or being exhaled. The Delta virus can reproduce itself so rapidly that our antibodies can't slow it down much. So vaccinated people shed viruses at a rate similar to unvaccinated people.
What you don't hear much about is the killer T-cells. The vaccines (or prior infection) also create trained T-cells. It appears that it's the second dose of the mRNA vaccines that activate the T-cells the most. They attach and kill our infected cells, preventing them from allowing the virus to replicate. Those cells are a lost cause anyway, and the body will eventually replace them. T-cells do not protect against getting infected; they only mitigate severity once infected. That's one-way vaccines limit the severity of the disease. That's why we don't see proportionally many vaccinated people with breakthrough infections among the hospitalized compared to the unvaccinated.
A new study found that even if vaccinated people get a breakthrough infection, they have a 49% lower risk of developing long-haul Covid. Symptoms of long-haul Covid can last for weeks to months to even longer. They include brain fog, fatigue, persistent loss of smell or taste, hair loss, and numbness.
Unfortunately, most vaccinated people mistakenly believe the vaccines protect them from infection, which they don't. They interpret vaccination as carte blanche to return to pre-pandemic life without restriction. They don't think they need to wear masks to protect themselves, so they can expose themselves to massive viral loads that overwhelm their immune systems. Unfortunately, the government, especially the CDC, has done a lousy job explaining the meaning of vaccination, which is probably responsible for most breakthrough infections.
Vaccinated people can have asymptomatic infections. So, for a group of only vaccinated people together who are unmasked, if one is asymptomatically infected and the group is together in close proximity, or in a riskier environment, such as a smaller indoor room, and they are together long enough, and even if social distancing, some can get infected if their viral load gets too high. One of the principal ways for Delta to spread is through aerosols that stay suspended in the air. Delta aerosols have much higher viral counts than the original coronavirus.
How Covid exposure works for the unvaccinated
If an unvaccinated person gets exposed to Covid, all they have is their innate immune system to fight it, which takes minutes to hours to kick in. That's the immune system you're born with. It includes physical barriers, such as skin and mucous membranes, and special cells and proteins that recognize and kill germs and viruses. However, the innate system produces far fewer antibodies and not the specialized antibodies that the vaccines produce. An unvaccinated person's immune system might eventually make a more robust response to the virus, but that process could take weeks. By then the virus may have caused a lot of harm and result in serious illness, long-term damage, or even death.
With the highly infectious nature of Delta (it reproduces very rapidly in the body, overwhelming the body's defenses) and the higher viral load it has in droplets and aerosols, an unvaccinated person's innate immune is not a strong defense against a Delta infection and the infection that can get serious.
A good way to measure how well the vaccines are working is the relative risk of Covid infection for vaccinated and unvaccinated people. By comparing the risk (rate of disease) among vaccinated people and unvaccinated people of the same age, we find that the risk of catching Covid-19, being hospitalized, or dying is far higher for people who are not fully vaccinated relative to vaccinated people. Here are the calculations from King County, WA during the 30 days before 8/27/2021.
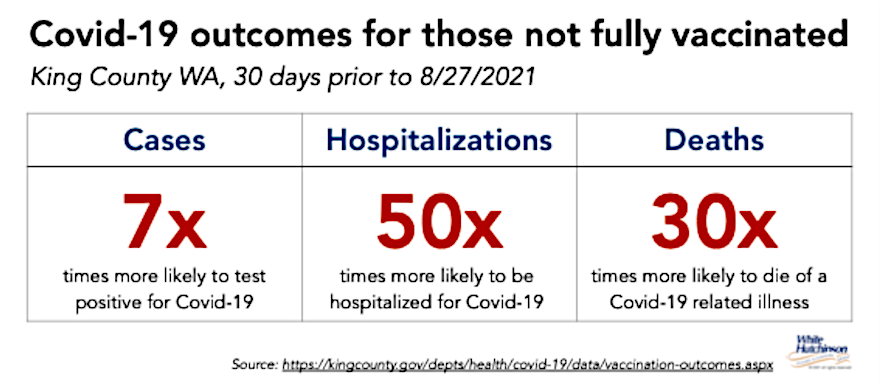
An added benefit of vaccination
In a new study published in the journal PLoS One, researchers tracked people who received the first dose of any coronavirus vaccine between December 2020 and March 2021. They found that those who had received a shot experienced significant improvements in their mental health, as they were less likely to show signs of mild or severe depression than those who had not been vaccinated, including those who intended to get vaccinated but had not yet been able to.
Mask protection
Masks can be very effective at stopping the transmission of droplets. However, when it comes to the transmission of aerosols, research by the University of Waterloo found that most common cloth masks, primarily due to problems with fit, filter only about 10% of exhaled aerosol droplets. The remaining aerosols are redirected, mainly out the top of the mask where it fits over the nose, and escape into the ambient air unfiltered.
By contrast, higher-quality, more expensive N95 and KN95 masks filter more than 50% of the exhaled aerosols that can accumulate indoors and spread the Covid-19 virus when inhaled by other people.
N95 masks, if properly fitted, prevent at least 95% of airborne particles from entering. Cloth masks are not very effective. The EPA found that a three-layer knitted cotton mask blocked 26.5% of particles, and a two-layer nylon mask with a filter insert and a metal nose bridge blocked 79%.
The problem with cloth masks is there are no standards governing them, so there is no way to know whether the particular one you're using is offering robust protection or not. This is why organizations have decided to ban them in favor of medical masks, which are subject to government regulations. Many airlines now ban cloth masks on flights, including Finnair, Air France, Lufthansa, Swissair, Croatia Airlines, and LATAM.
A recent study among more than 350,000 adults living in 600 rural communities in Bangladesh found that medical masks, such as N95s, prevented one in three (35%) symptomatic infections among unvaccinated community members 60 years and older.
Bi-weekly tests in lieu of vaccination
Some companies are giving employees the option of getting tested for Covid twice a week instead of getting vaccinated. That is really a foolish approach for protecting other employees and customers from infection. Tests will not detect an infection until 3 to 5 days after the initial infection. Once someone has symptoms or Delta infection is detected, the infected person already has viral loads over 1,000 times higher than the original strain of coronavirus, making them highly contagious. They are most contagious, shedding the greatest amount of Delta virus, 1 or 2 days before testing positive or feeling sick. During that time, they could easily have been infecting others for several days. Nearly three-quarters of infections from Delta happen during the pre-symptomatic phase.
So, bi-weekly testing will not identify an infected person until several days after they were contagious and likely spreading the virus to other employees and customers.
The bottom line
To significantly reduce your chances of getting infected with the Delta variant and protecting yourself from getting seriously ill, ending up in the hospital, or even death, or spreading it to loved ones, you need to get fully vaccinated. Regardless of whether you are vaccinated or unvaccinated, you should wear a well-fitted medical mask when out in public (even among all vaccinated people) as both vaccinated and unvaccinated people can be asymptomatically infected and spread the infection to others. This includes vaccinated people who can get a breakthrough infection
Mask mandates
The majority of people feel safer visiting a business if everyone is wearing a mask. A mid-August Axios/Ipsos poll found that two-thirds of adults (64%) support governmental mandates requiring masks to be worn in all public places.
For businesses, all staff and all customers should be mandated to wear masks. This is especially important due to the shortage of workers. The last thing a business needs right now is to have a significant number of staff get infected and be quarantined.
Vaccine mandates
The vaccine status of employees is also important to consumers. A mid-August Harris Poll found over half of Americans (53%) reported they are more likely to shop in-store at companies that require their employees to be vaccinated. About half say they're more likely to shop in-store if customers are required to be vaccinated. Younger consumers are most likely to base in-store decisions on vaccine mandates, with 56% of Gen Zers saying so.
The survey also found that three-quarters of consumers (76%) agree that companies who require employee vaccinations should make that fact explicit in their advertising. Over two-thirds agree (69%) that consumers have a right to know whether a company requires vaccinations of its employees.



